
8 surprising facts about sepsis everyone should know
Sepsis is a condition that results from the body’s overwhelming and life-threatening response to an infection that can lead to tissue damage, organ failure and death. Recently HAP’s Dr. Peter Watson, vice president of clinical operations and strategy, spoke to Dr. Namita Jayaprakash, who leads the Sepsis Program for Henry Ford Health, about the dangers of sepsis and why everyone should learn about this important health risk.
For Dr. Jayaprakash, sepsis is a very common condition she faces with her patients both in the emergency department and the medical intensive care unit.
“Sepsis occurs when the body's immune response goes out of balance in the healing process, and the result is a triggering of changes that can damage multiple organ systems,” Dr. Jayaprakash notes. “So, sepsis can be the result of any infection. And yes, it is a more serious condition because it can be life threatening when organ systems are damaged.”
She offered these eight key facts everyone should know:
- It’s common and very risky: Sepsis is a major public health threat. With over 19 million cases each year worldwide, sepsis accounts for 1 in 10 of all intensive care unit (ICU) admissions. Risk for death from sepsis in hospitalized patients can range from 30-50%.
- There are warning signs: Infection occurs when viruses, bacteria or other microbes enter the body and start to damage the body’s cells. Signs and symptoms of the infection appear as an illness and cause us to feel unwell. In response to an infection, our body’s immune system springs into action and releases a defense mechanism into the bloodstream to fight the infection.
- It can be deadly: More than 1.7 million people in the U.S. are diagnosed with sepsis each year, which is 1 every 20 seconds. Sepsis remains the leading cause of death in U.S. hospitals.
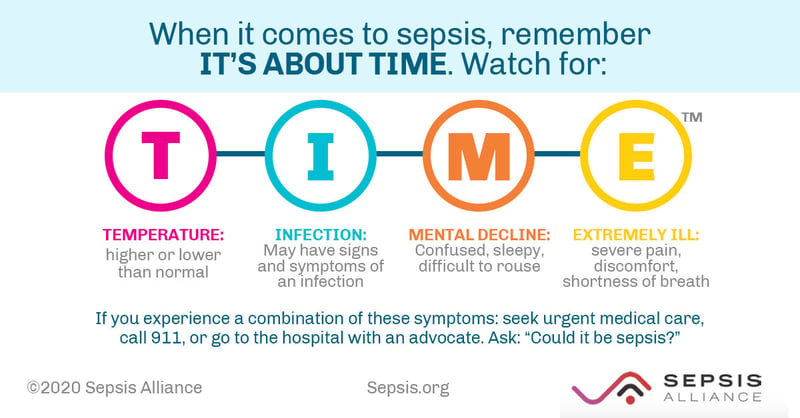
- There are key symptoms: A good way to think about some of the symptoms that may indicate sepsis is to use the acronym T.I.M.E.
T = Temperature change
I = Infection
M = Mental status changes
E = Extremely ill
- Factors toward diagnosis: Doctors diagnose sepsis by putting together the story, physical examination findings and sometimes even laboratory blood tests and x-rays. They look for:
- Fever
- Low blood pressure
- Increased heart rate
- Signs that suggest difficulty with breathing
- Confusion or changes in level of alertness
- Several treatment options: Sepsis is a medical emergency and should be treated as quickly and efficiently as possible. The clock starts as soon as sepsis is identified. The key to treatment of sepsis is the rapid administration of antimicrobials while also getting cultures and finding the source to control it.
- Who is at risk? The very young and the elderly are most susceptible to sepsis.
- Sepsis can be avoided: Knowledge is power in identifying sepsis. Having awareness of the severity of the illness and seeking help when you are worried about sepsis is key.
Dr. Jayaprakash also offers these steps to help avoid sepsis: They include:
- Stay up to date on age-appropriate CDC vaccinations.
- Be vigilant about managing chronic conditions that put you at greater risk of infection such as diabetes, heart disease and lung conditions.
- Practice good hygiene: Hand washing is a great strategy for preventing infections – we saw this with COVID-19, for example. Masks help reduce the transmission of infections.
- Care for any skin injuries to avoid wound infections.
- Be aware of the signs of early infection and work with your primary care physician for early diagnosis, monitoring and treatment.
- Staying on top of your nutrition and thinking about ways to maintain a balanced diet can also be a key strategy.
There are many treatment options used to fight sepsis, including rapid administration of antimicrobials, fluids, oxygen and IV medications.
Visit hap.orgto learn more about other topics. As always, HAP is here to help you understand and better manage your own health and well-being.
Categories: Get Healthy, Get Involved