
Understanding Your Member ID Card: What All Those Numbers Mean
Your HAP member ID card is your ticket to medical care. It identifies you and lets your doctors and other providers know how to submit your claims. Here’s how it works.
Who gets an ID card?
Primary members, their spouses and dependents age 18 and older get cards. HAP does not send physical ID cards to members under 18 years of age.
All members, including dependents under 18, can access a digital ID card. These are available via our HAP OnTheGo mobile app or by logging in at hap.org. When taking children under 18 for services, parents should show their own card. Or, they can show their child’s digital ID card.
What does the information on my card mean?
Your member ID card contains two types of information. On it, you’ll find:
- The contacts you may need to call for help or information.
- Some numbers that identify your plan or coverage. Those numbers give your doctor’s office or pharmacist the information they need to file a claim for your care.
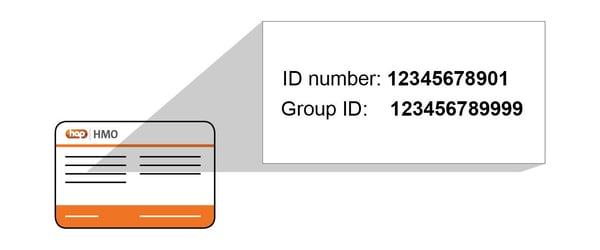
Here’s what they all mean:
ID number - Identifies you as a HAP member and is the primary information providers use to get claims processed. It’s also the number you'll use to register at your hap.org account.
Group ID - How we identify your employer group, if you have health coverage through work.
Prescriptions are processed through a company that administers HAP’s drug benefits. This company is called a pharmacy benefits manager or PBM. Rx is short for prescription. The Rx numbers on your card tell your pharmacy how to process your claim so your prescriptions get paid correctly.
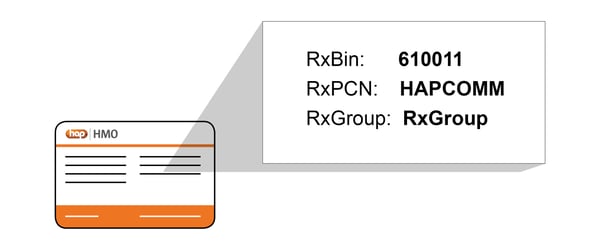
RxBin - Stands for bank identification number, but it doesn’t actually involve a bank. It’s the number that tells the pharmacy database which PBM should receive your claim.
RxPCN - Stands for processor control number. It’s another number used to locate your pharmacy member profile under the PBM system.
RxGroup - Each PBM has many groups. This number tells the pharmacy which group you’re in so they can process your prescription payment correctly.
RxID - For members who have Medicare part D, this is your pharmacy member number in the PBM’s system. It’s used to allow the pharmacist to process claims.
Your card also has information about the type of plan you have and your provider network.

Plan type - At the top of your card you’ll see something that may say HMO, PPO, etc. This is the type of plan you have. Click here to learn more about plan types.
Network - This is the group of doctors and hospitals you can go to for care. To find a provider in your network, log in at hap.org and click on Find a Doctor/Facility and then click on Search for a Doctor or Facility.
Tiered access - If you have a tiered network, you might have different out-of-pocket costs for providers in the different tiers. When you log in at hap.org and search for a provider, if you have a tiered network, each provider will list which tier they are in. Click here to read more about tiered networks.
![]()
Any time you get a new card in the mail, be sure to start using it and destroy your old card so you have the most current plan info at your fingertips and to make sure your claims are paid correctly.
If you need an additional card, log in to your hap.org account and request one to be mailed, or download one to use immediately. If you have questions about your coverage, please call a Customer Service specialist at the number on your HAP ID card.
Categories: Get To Know Your Plan
Tags: Blog